Wednesday, May 18, 2016
Bone density and avoiding Osteoporosis / Osteopenia in severe M.E / CFS
If you have severe M.E or any type of long term illness it's worth thinking about bone density.
My experience
A friend with severe M.E was diagnosed with severe Osteoporosis at the age of 21, I was 25 at the time and immediately asked if I could be tested. My consultant told me to expect it to show Osteoporosis and my GP referred me for a DEXA scan. It showed I was at high risk of fractures, especially hip ones. With treatment a follow up scan showed my bone density had improved, I am sure if it hadn't been for my friends diagnosis my bone density would still be getting worse. I posted on Facebook and several other people went to get tested.
Risk factors
Risk factors include poor diet, low weight, low vitamin D, long term steroids and not weight bearing. At various points over the years I've met all those criteria and yet no doctor had ever raised the possibility of bone loss.
Testing
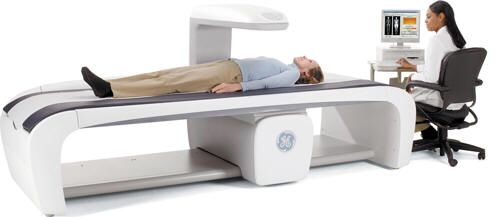
Aside the traveling aspect the actual test is fine. They can either do a DEXA scan or an X-ray of your heel bone although I'm told the results aren't as accurate of the heel bone as the DEXA. For the first part I had my hip scanned, I laid on my back and they strapped my foot turned inwards to give the best position of my hip for the scan. As my feet naturally turn inwards these days this was pain free and the scan didn't take long. Next they put a block under my knees so my spine would be flatter, again as I lay with my legs up normally this was fairly comfortable. The arm moved up and down my spine and took about 10 minutes. It's not noisy or claustrophobic at all and doesn't touch you. You don't need to get undressed or changed into a gown for the scan.
I also had bone profile blood tests done and vitamin D
A picture of a DEXA scan
Treatment
I was started on massive doses of Vitamin D and also calcium (both prescribed) and given a physio plan. Although standing and walking is clearly best I was given tiny exercises to do through out the day like pushing my knee into the bed or foot against the footboard, anything to add a little resistance through my bones. We also discussed starting on the pill as Oestrogen can help but I decided against this. There are also drugs (Including oral or IV) for Osteoporosis but we decided to wait and rescan with just vit d/calcium/physio.
I rang The National Osteoporosis Society helpline and spoke to a nurse who was very helpful and sent me some information in the post. I obviously knew the old advice to drink milk (although I know some disagree with that) but they told me about things like research that eating prunes can help and about the different drug options. Their site is full of information www?not.org.uk
I would add that you don't need to have osteoporosis/osteopenia or scans to start treatment. Prevention is really important and if I could go back in time I would work on this from day 1 of becoming severe. I asked my physio of what kind of duration of being bed bound would bone density start becoming a problem, she said the honest answer is she doesn't know, even as professionals it's not something they tend to think about in young people.
For more help on preventing or treating bone density problems see here
Saturday, December 19, 2015
Tuesday, December 15, 2015
Donating toys and gifts to children in hospital
This was written by someone I know who is a doctor. I run a charity for seriously ill children and can grant most wishes for young cute kids with cancer and provide 10 different holidays but it's much harder for other conditions!
Sent from my iPhone
Last year I worked in a children's hospital at Christmas time, and there were so many presents donated, mostly from corporate donors. The entire large meeting room was taken over with gifts to sort. There were hundreds too many presents, so some were leftover for birthdays and other occasions. We still had boxes full of Lego packs in June.
This Christmas I'm working in child and adolescent mental health, still in a hospital ward. We have had no presents donated and I don't imagine we're going to. Our patients will have one present each, chosen by the therapy team, paid for out of the ward's budget - scrimped and saved from the budget that is meant to cover food, activities, and other expenses.
If your company, or RAG society, or someone you know is thinking of donating gifts to the poorly children in hospital this Christmas, ask them to donate them to the poorly children in the mental health hospitals instead. They're not as cute and photogenic and good for corporate image, but they're less likely than a sick kid in a medical hospital to have loving family showering them with gifts. Any gifts to child and adolescent mental health services (CAMHS) would be appreciated, both by the young people, and by the staff trying to stretch the budgets to give the patients a nice time.
It would be lovely if the world could start to address the stigma of mental health, and the disparity of only caring about children with physical problems rather than also those with mental problems.
EDIT: This is the link to the list of CAMHS wards in alphabetical order. They aren't all NHS, but even the private ones will have lots of NHS patients because of CAMHS underfunding and bed crisis. http://www.rcpsych.ac.uk/workinpsychiatry/qualityimprovement/ccqiprojects/childandadolescent/inpatientcamhsqnic/membersdirectory.aspx?theme=mobile
This link shows you CAMHS units on a map, by region, but doesn't seem to work from a mobile http://www.rcpsych.ac.uk/workinpsychiatry/qualityimprovement/ccqiprojects/childandadolescent/inpatientcamhsqnic/mappingofcamhsunits.aspx
This link shows you CAMHS units on a map, by region, but doesn't seem to work from a mobile http://www.rcpsych.ac.uk/workinpsychiatry/qualityimprovement/ccqiprojects/childandadolescent/inpatientcamhsqnic/mappingofcamhsunits.aspx
Good generic presents include things for an older child or teenager: arts and crafts things, colouring books, cookery things (my patients love cooking and baking!), remote control cars and helicopters, nail varnish, age-appropriate DVDs, nice smellies. Nothing sharp or that could easily break.
Corporate or larger gifts for a CAMHS ward would include games consoles, sports equipment, cooking equipment (smoothie maker?!), a TV or radio - but best to consult with the ward you're donating to.
Cards would also go down well, even if it just says eg "to young people and staff at [hospital], seasons greetings"
Sent from my iPhone
My Christmas gift creations
I've been planning lots of blog entries but never seem to get around to writing them. I wanted to share some of the Christmas gifts I've made this year and also some gift ideas. I've been busy crafting but I've only been doing small projects which can be done in bed, hoping to start baking next week though!
First up we have this decoration for my friend Cat. I've blogged in the past about the cream decorations I had purchased from Dot Com Giftshop but wasn't too keen on when I saw them in real life. This year I found a nail varnish in my friends favourite colour and set about painting with it hoping for a result like the gold ones last year. To say it didn't go well would be an understatement, it looked mouldy! We decided that maybe Mouldy Chic is the new Shabby Chic but thankfully after several more coats it no longer looked mouldy although it wasn't the colour I had hoped for.

Next up is a sugar free alternative to a sweet cone or hot chocolate cone. My friend is dairy, gluten and gelatine free so needs a healthy alternative to a sweet cone. I got some red skinned peanuts and cashew nuts as she likes both. I first planned to make a Santa head by filling the majority cone with red nuts and then a circular shape with the cashews. My plan was to turn it upside down, add a white pom-pom to the top of the 'hat' and add wiggly eyes. I changed my mind and decided to go for a candy cane style stripe with the 2 nuts.

Next up is a gift I got for most of my friends. Each year I get ornaments made from Artscow, never buy straight from their site as they do mega discount codes if your patient enough to wait. Often I go for photographs relating to the person or quotes, this year it's Harry Potter quotes. Harry Potter is full of fantastic quotes but 2 of my favourites are 'It is not our abilities that define us, it is our choices' and 'happiness can always be found in the darkest times, if someone only remembers to turn on a light'. I selected the background, colour and font and got them delivered to me. They arrive on red ribbon which I think looks cheap and they look much better after switching to a coordinating coloured ribbon.
Before and after ribbon change


As little stocking fillers I had some personalised glass cloths printed. I used different pictures for different people and added text to some of them. These are for my family and cost me a grand total of 63p each including shipping!

I've made snowmen and snowflake Oreo pops for people as a 'Happy 1st December' gift. I wrapped them in cellophane and put a Christmas sticker on the back to neaten things.

I've been working on this Design Works cushion for ages but it's so difficult to sew the buttons on as the material is thick and the needle is thick and blunt! I don't think I'm going to get it finished in time.
Not so much handmade but I've put together a selection of After Eight Mints for my Grandpa. He doesn't like much these days but these are the one thing he does still like. They now do straws and segments so I got those and also some normal ones for us to play with. Last year we did the challenge when you tilt your head back, place the mint on your forehead and use your muscles to wiggle it down to your mouth. HINT if you want to cheat make sure you warm the other persons one slightly! I discovered this as I was hot and while everyone else managed to do there's mine was still on my forehead (not helped but us all having uncontrolled hysterics!). I even leant forwards and it remained stuck to my head!

Earlier in the year I made this for some newly weds. It's for their first Christmas tree as a married couple.

Last but not least a close up video of the stockings I've been working on for a few years (yet to be fully finished!).
First up we have this decoration for my friend Cat. I've blogged in the past about the cream decorations I had purchased from Dot Com Giftshop but wasn't too keen on when I saw them in real life. This year I found a nail varnish in my friends favourite colour and set about painting with it hoping for a result like the gold ones last year. To say it didn't go well would be an understatement, it looked mouldy! We decided that maybe Mouldy Chic is the new Shabby Chic but thankfully after several more coats it no longer looked mouldy although it wasn't the colour I had hoped for.

Next up is a sugar free alternative to a sweet cone or hot chocolate cone. My friend is dairy, gluten and gelatine free so needs a healthy alternative to a sweet cone. I got some red skinned peanuts and cashew nuts as she likes both. I first planned to make a Santa head by filling the majority cone with red nuts and then a circular shape with the cashews. My plan was to turn it upside down, add a white pom-pom to the top of the 'hat' and add wiggly eyes. I changed my mind and decided to go for a candy cane style stripe with the 2 nuts.

Next up is a gift I got for most of my friends. Each year I get ornaments made from Artscow, never buy straight from their site as they do mega discount codes if your patient enough to wait. Often I go for photographs relating to the person or quotes, this year it's Harry Potter quotes. Harry Potter is full of fantastic quotes but 2 of my favourites are 'It is not our abilities that define us, it is our choices' and 'happiness can always be found in the darkest times, if someone only remembers to turn on a light'. I selected the background, colour and font and got them delivered to me. They arrive on red ribbon which I think looks cheap and they look much better after switching to a coordinating coloured ribbon.
Before and after ribbon change


As little stocking fillers I had some personalised glass cloths printed. I used different pictures for different people and added text to some of them. These are for my family and cost me a grand total of 63p each including shipping!

I've made snowmen and snowflake Oreo pops for people as a 'Happy 1st December' gift. I wrapped them in cellophane and put a Christmas sticker on the back to neaten things.

I've been working on this Design Works cushion for ages but it's so difficult to sew the buttons on as the material is thick and the needle is thick and blunt! I don't think I'm going to get it finished in time.

Not so much handmade but I've put together a selection of After Eight Mints for my Grandpa. He doesn't like much these days but these are the one thing he does still like. They now do straws and segments so I got those and also some normal ones for us to play with. Last year we did the challenge when you tilt your head back, place the mint on your forehead and use your muscles to wiggle it down to your mouth. HINT if you want to cheat make sure you warm the other persons one slightly! I discovered this as I was hot and while everyone else managed to do there's mine was still on my forehead (not helped but us all having uncontrolled hysterics!). I even leant forwards and it remained stuck to my head!

Earlier in the year I made this for some newly weds. It's for their first Christmas tree as a married couple.

Last but not least a close up video of the stockings I've been working on for a few years (yet to be fully finished!).
Monday, December 14, 2015
Oreo Snowmen (head and body) and Oreo Snowflake Pop tutorial
I've been busy making Oreo snowmen and Oreo snowflake pops.
I've seen lots of Oreo snowmen heads but they never have a body. I did a search and still couldn't find any although I did find these adorable snowmen heads.

I decided to have a go at making some using normal Oreo's and mini ones (from snack packs) but quickly learnt the key to good looking Oreo pops is doubled stuffed ones.
To make these snowmen you need,
Double stuff Oreo's
Snack packs of Oreo's
Lollipop or cake pop sticks
Candy melts
Things to decorate with.

Start by gently separating the 2 halves of the both the double stuff and mini Oreo's, be prepared for plenty of breakages, you can either 'glue' them back in place or enjoy eating them (would be awful to let them go to waste...).

Take the mini Oreos and using the candy melts 'glue' the top of the stick into them. You don't want to have any of the stick poking out of the top. 'Glue' the other half on.
Make a dent in the 'stuffing' of the larger Oreo, before 'gluing' the stick in and adding the other half on top. You want the big Oreo and mini Oreo to touch.

Put the Oreo's on sticks in the fridge for a few minutes to firm or have a cup of tea while enjoying the broken ones.
Dip the Oreo's on the stick in the candy melts, it helps if you add Trex/shortening to the candy as it will make a smoother coating. Stand them up to dry, I used a block of polystyrene but anything like that will work. When dry do a second coat then decorate.

These were decorated with coloured pearls and little tubes of writing icing.


Wrap in cellophane or eat straight away!

I've seen lots of Oreo snowmen heads but they never have a body. I did a search and still couldn't find any although I did find these adorable snowmen heads.

I decided to have a go at making some using normal Oreo's and mini ones (from snack packs) but quickly learnt the key to good looking Oreo pops is doubled stuffed ones.
To make these snowmen you need,
Double stuff Oreo's
Snack packs of Oreo's
Lollipop or cake pop sticks
Candy melts
Things to decorate with.

Start by gently separating the 2 halves of the both the double stuff and mini Oreo's, be prepared for plenty of breakages, you can either 'glue' them back in place or enjoy eating them (would be awful to let them go to waste...).

Take the mini Oreos and using the candy melts 'glue' the top of the stick into them. You don't want to have any of the stick poking out of the top. 'Glue' the other half on.
Make a dent in the 'stuffing' of the larger Oreo, before 'gluing' the stick in and adding the other half on top. You want the big Oreo and mini Oreo to touch.

Put the Oreo's on sticks in the fridge for a few minutes to firm or have a cup of tea while enjoying the broken ones.
Dip the Oreo's on the stick in the candy melts, it helps if you add Trex/shortening to the candy as it will make a smoother coating. Stand them up to dry, I used a block of polystyrene but anything like that will work. When dry do a second coat then decorate.

These were decorated with coloured pearls and little tubes of writing icing.


Wrap in cellophane or eat straight away!

Thursday, July 30, 2015
Meerkat Madness!
Yes that's a Meerkat and yes it's in my mouth!

Someone then turned a photo into this!

Will blog soon about my annual day out of bed but thought I would share the meerkat moment (in case you are wondering, it was checking my ears and mouth for grubs, pleased to say that no grubs were located in me).
Final picture of my annual day out with Holly


Someone then turned a photo into this!

Will blog soon about my annual day out of bed but thought I would share the meerkat moment (in case you are wondering, it was checking my ears and mouth for grubs, pleased to say that no grubs were located in me).
Final picture of my annual day out with Holly

Wednesday, May 27, 2015
Perfect Party UK Balloons
My day to day name is Vikki but my not so secret identity is The Balloon Fairy.

A picture of me about to release some balloon with forget-me-not seeds inside in memory of some children who sadly passed away
Perfect Party UK are asking bloggers to blog about balloons, as you will know if you saw my balloon fairy blog a couple of years ago I LOVE balloons.
My earliest balloon memories are of discos held in a school hall. There would also be a big net over the ceiling full of balloons, the highlight of the disco would be when the net let down the balloons and we would all desperately try and get a pretty marble one or a long wiggly one!
My love of balloons has never faded and we keep a party canister of helium in our garage. Next week it's my Mums birthday, shortly followed by my Dads and then Father's Day. I have purchased some balloons and will secretly blow them up and tie them to bedroom door handles over night so the balloons are the first thing they see. My favourite balloons are either foil or bubble (bubble are made of a clear plastic which are thicker than your average latex balloon and apart from looking better they stay floating for a very long time). Its a cheap way of making a big impact, Perfect Party UK have a huge range all under £3 each!
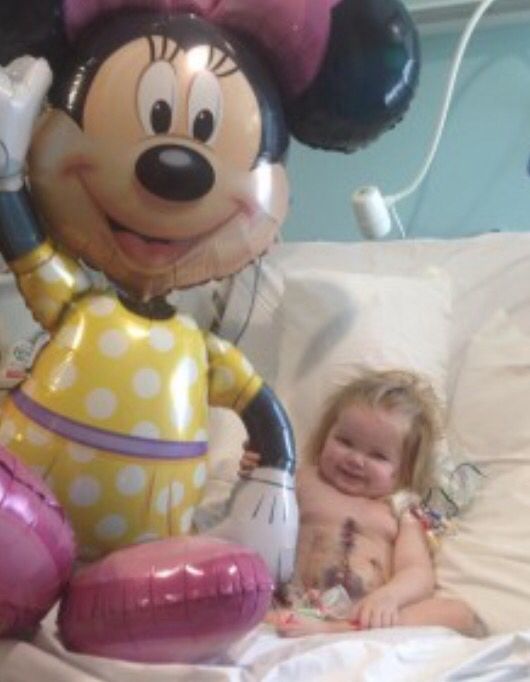
It might be a tad sad but I have spent countless hours researching different balloons so I can find the perfect balloons for occasions or people and I'm pleased to say Perfect Party UK stock my top 3! Check out these airwalkers, Spider-Man who when filled looks like he is climbing on the ceiling and a giant Minnie and Mickey. I sent Minnie to a little girl following her second kidney transplant, do you think she liked it?
So you get that I like balloons but why am I The Balloon Fairy? I will copy this from my previous blog entry;
'I love balloons, they can mean celebration, happiness, get well or good luck wishes, congratulations, sad goodbyes and even 'just because'.
I had some helium left over recently and so today we blew up some balloons. My original plan was to do some and have Mum tie them to the front door of a neighbour (who has the same illness as me) with a note just saying they were from the balloon fairy. I realised it was her 18th birthday this week though so blew up lots of balloons which mum took up with a card. This isn't the first time there has been a balloon fairy. A few years back when I was doing better, I managed to go to a dinner organised by the local paper and they presented organisations/charities with a donation. As soon as I entered the room I clocked the heart balloon bouquets and thought of how they could make kids smile. I was able to ask an official if it would be possible to take some home to give to some local children, they said they would find out for me. So we have dinner, then the cheques are presented and everyone was moved so I could join the others for a photo at the front of the room. After it had been taken they announced that children's charities can take the balloons and to my horror they all seemed to instantly vanish before me (all the other charity people could walk!) and there was chaos trying to move me an inch forward. I told my dad 'forget me, the balloooons, the balloooons' (seriously, anyone would think they had bunches of winning lottery tickets rather than some heart shaped balloons), some kind guy over heard me and snagged me quite a few. Everyone who was with me pointed out we could never get that many balloons in our car and I informed them that they should be positive and when there is a will there is a way (I'm not sure if positivity effects the laws of physics but hey it's worth a try). My dad had recently got a new car which didn't have a boot the size of his old one (which got mentioned every time the boot was used) and my wheelchair alone filled it. That left 4 of us and about 18 balloons, we had them crammed into every nook and cranny, I even had my leg over some so they wouldn't obstruct Dads view, thank god it was dark! We concluded that if we were in an accident we would be fine due to this very large air cushion surrounding us but when rescued we would be all squeaky as its helium! My insanity paid off though, the next day balloons were delivered to a boy who had recently seen his sister die and a family where a mixture of illness and disability led the family to crisis point, they got home to find their porch filled with balloons from seemingly no where (although they guessed it was us). The kids apparently loved it and decided it was the balloon fairy!'


A picture of me about to release some balloon with forget-me-not seeds inside in memory of some children who sadly passed away
Perfect Party UK are asking bloggers to blog about balloons, as you will know if you saw my balloon fairy blog a couple of years ago I LOVE balloons.
My earliest balloon memories are of discos held in a school hall. There would also be a big net over the ceiling full of balloons, the highlight of the disco would be when the net let down the balloons and we would all desperately try and get a pretty marble one or a long wiggly one!
My love of balloons has never faded and we keep a party canister of helium in our garage. Next week it's my Mums birthday, shortly followed by my Dads and then Father's Day. I have purchased some balloons and will secretly blow them up and tie them to bedroom door handles over night so the balloons are the first thing they see. My favourite balloons are either foil or bubble (bubble are made of a clear plastic which are thicker than your average latex balloon and apart from looking better they stay floating for a very long time). Its a cheap way of making a big impact, Perfect Party UK have a huge range all under £3 each!
It might be a tad sad but I have spent countless hours researching different balloons so I can find the perfect balloons for occasions or people and I'm pleased to say Perfect Party UK stock my top 3! Check out these airwalkers, Spider-Man who when filled looks like he is climbing on the ceiling and a giant Minnie and Mickey. I sent Minnie to a little girl following her second kidney transplant, do you think she liked it?

So you get that I like balloons but why am I The Balloon Fairy? I will copy this from my previous blog entry;
'I love balloons, they can mean celebration, happiness, get well or good luck wishes, congratulations, sad goodbyes and even 'just because'.
I had some helium left over recently and so today we blew up some balloons. My original plan was to do some and have Mum tie them to the front door of a neighbour (who has the same illness as me) with a note just saying they were from the balloon fairy. I realised it was her 18th birthday this week though so blew up lots of balloons which mum took up with a card. This isn't the first time there has been a balloon fairy. A few years back when I was doing better, I managed to go to a dinner organised by the local paper and they presented organisations/charities with a donation. As soon as I entered the room I clocked the heart balloon bouquets and thought of how they could make kids smile. I was able to ask an official if it would be possible to take some home to give to some local children, they said they would find out for me. So we have dinner, then the cheques are presented and everyone was moved so I could join the others for a photo at the front of the room. After it had been taken they announced that children's charities can take the balloons and to my horror they all seemed to instantly vanish before me (all the other charity people could walk!) and there was chaos trying to move me an inch forward. I told my dad 'forget me, the balloooons, the balloooons' (seriously, anyone would think they had bunches of winning lottery tickets rather than some heart shaped balloons), some kind guy over heard me and snagged me quite a few. Everyone who was with me pointed out we could never get that many balloons in our car and I informed them that they should be positive and when there is a will there is a way (I'm not sure if positivity effects the laws of physics but hey it's worth a try). My dad had recently got a new car which didn't have a boot the size of his old one (which got mentioned every time the boot was used) and my wheelchair alone filled it. That left 4 of us and about 18 balloons, we had them crammed into every nook and cranny, I even had my leg over some so they wouldn't obstruct Dads view, thank god it was dark! We concluded that if we were in an accident we would be fine due to this very large air cushion surrounding us but when rescued we would be all squeaky as its helium! My insanity paid off though, the next day balloons were delivered to a boy who had recently seen his sister die and a family where a mixture of illness and disability led the family to crisis point, they got home to find their porch filled with balloons from seemingly no where (although they guessed it was us). The kids apparently loved it and decided it was the balloon fairy!'

Subscribe to:
Posts (Atom)